HSC-2 Xenograft Model Overview
The HSC-2 xenograft model is derived from a well-established human oral squamous cell carcinoma (OSCC) line, originally isolated from the tongue of a 69-year-old male patient. As a model of differentiated OSCC, HSC-2 xenografts closely replicate the pathological and molecular characteristics of human oral cavity cancers. This model is commonly employed in translational research on chemoradiotherapy resistance, epithelial–mesenchymal transition (EMT), and targeted therapy development. The tumors exhibit consistent in vivo growth kinetics and histological features of keratinizing squamous cell carcinoma, making HSC-2 a robust platform for studying tumorigenesis, oral mucosal biology, and therapeutic modulation in head and neck oncology.
Request a Custom Quote for HSC-2 Xenograft ModelBiological and Molecular Characteristics
HSC-2 cells display cobblestone-like epithelial morphology and maintain features of moderately differentiated squamous cell carcinoma. The cell line is HPV-negative and demonstrates wild-type TP53, although functional p53 activity is diminished due to upstream regulatory changes. HSC-2 is characterized by moderate EGFR expression and elevated activity in the PI3K/AKT and MAPK signaling pathways. The model expresses classical cytokeratins (CK5, CK14) and exhibits partial responsiveness to EMT-inducing stimuli such as TGF-β, with upregulation of mesenchymal markers including N-cadherin and vimentin under specific conditions. Microsatellite status is stable (MSS), and there are no pathogenic mutations in KRAS, BRAF, or PIK3CA, providing a relatively stable genomic background for targeted intervention studies.
| Characteristic | HSC-2 Cell Line Profile |
|---|---|
| Tissue of Origin | Tongue squamous cell carcinoma |
| HPV Status | Negative |
| TP53 Status | Wild-type (functionally impaired) |
| EGFR Status | Moderate expression |
| MSI Status | Microsatellite stable (MSS) |
| EMT Induction | Partial (↑vimentin, ↑N-cadherin under TGF-β) |
In Vivo Model Development and Tumorigenicity
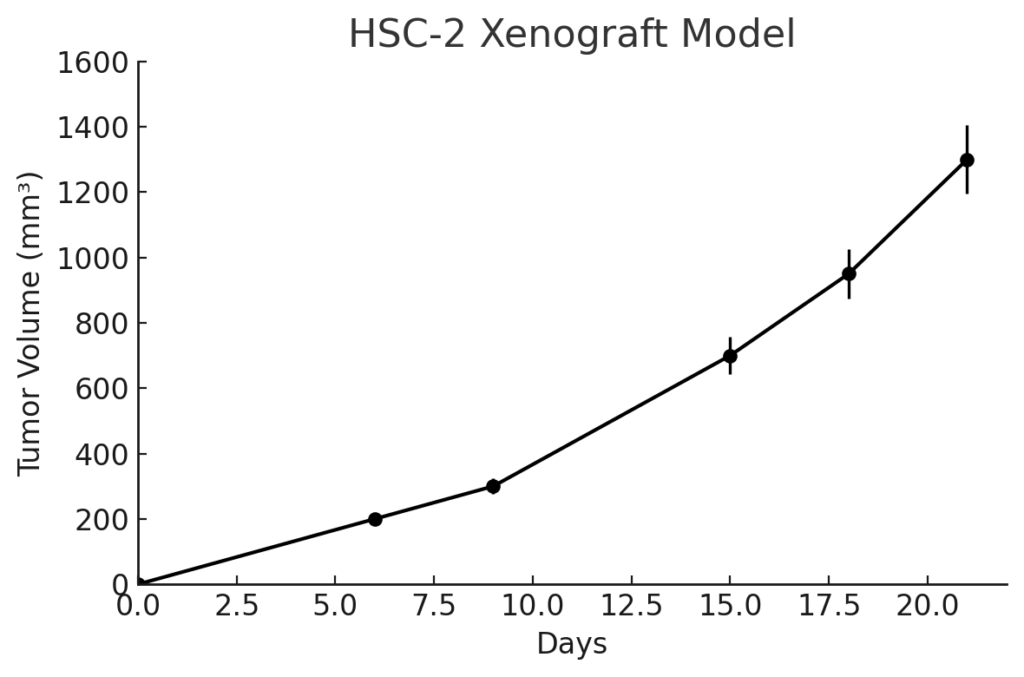
HSC-2 xenografts are established by subcutaneous injection of cultured tumor cells into immunodeficient mouse strains such as athymic nude or NOD/SCID mice. Tumor nodules typically appear within 7–10 days post-implantation and reach target volumes (700–900 mm³) within 4–5 weeks, with high take rates and predictable growth patterns. HSC-2 tumors exhibit moderately aggressive expansion and a well-differentiated histological phenotype, making them suitable for long-term studies assessing therapeutic response and tumor progression. The model has been employed in evaluating chemotherapy, radiotherapy, and biologically targeted agents, including those affecting EMT, EGFR, and DNA repair mechanisms in oral squamous carcinoma.
Request a Custom Quote for HSC-2 Xenograft ModelHistopathology and Immunohistochemical Profile
Histopathological evaluation of HSC-2 xenografts reveals well-organized squamous epithelial architecture with keratin pearl formation, prominent intercellular bridges, and moderate mitotic activity. Hematoxylin and eosin (H&E) staining confirms the keratinizing phenotype typical of differentiated OSCC. Immunohistochemical staining demonstrates positivity for cytokeratins CK5 and CK14, moderate EGFR expression, and variable nuclear p53 staining. Mesenchymal markers such as vimentin and N-cadherin are upregulated in xenografts treated with EMT-inducing agents or grown under hypoxic conditions. The absence of p16INK4a and lack of HPV E6/E7 protein expression further support the model’s HPV-negative classification.
Preclinical Applications and Drug Response
The HSC-2 xenograft model is widely used in preclinical studies targeting oral squamous cell carcinoma. It serves as an effective platform for evaluating standard therapies, including cisplatin, 5-fluorouracil, and radiation, as well as novel agents targeting EGFR, PI3K/AKT, and EMT-associated pathways. Its ability to partially undergo EMT under external stimuli makes it suitable for testing therapeutic compounds that reverse or inhibit mesenchymal transition. In addition, the HSC-2 model supports the development of topical or intraoral drug formulations due to its anatomical origin and mucosal relevance. It also contributes to the study of DNA repair inhibition, apoptosis modulation, and microenvironmental interactions in head and neck cancer research.
Request This Model
To incorporate the HSC-2 xenograft model into your oral cancer or head and neck oncology studies, please contact our team to receive full model specifications and expert guidance on customizing preclinical protocols for HPV-negative, EGFR-expressing squamous cell carcinoma.
Request a Custom Quote for HSC-2 Xenograft Model